In this episode, we discuss acute decompensated heart failure and how to best manage these dyspneic patients in the ED.

 Core EM - Emergency Medicine Podcast
Core EM - Emergency Medicine Podcast Episode 159.0 – Acute Decompensated Heart Failure
8 snips
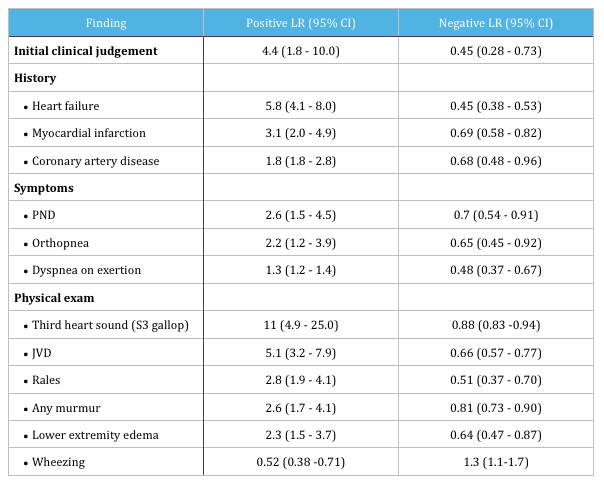
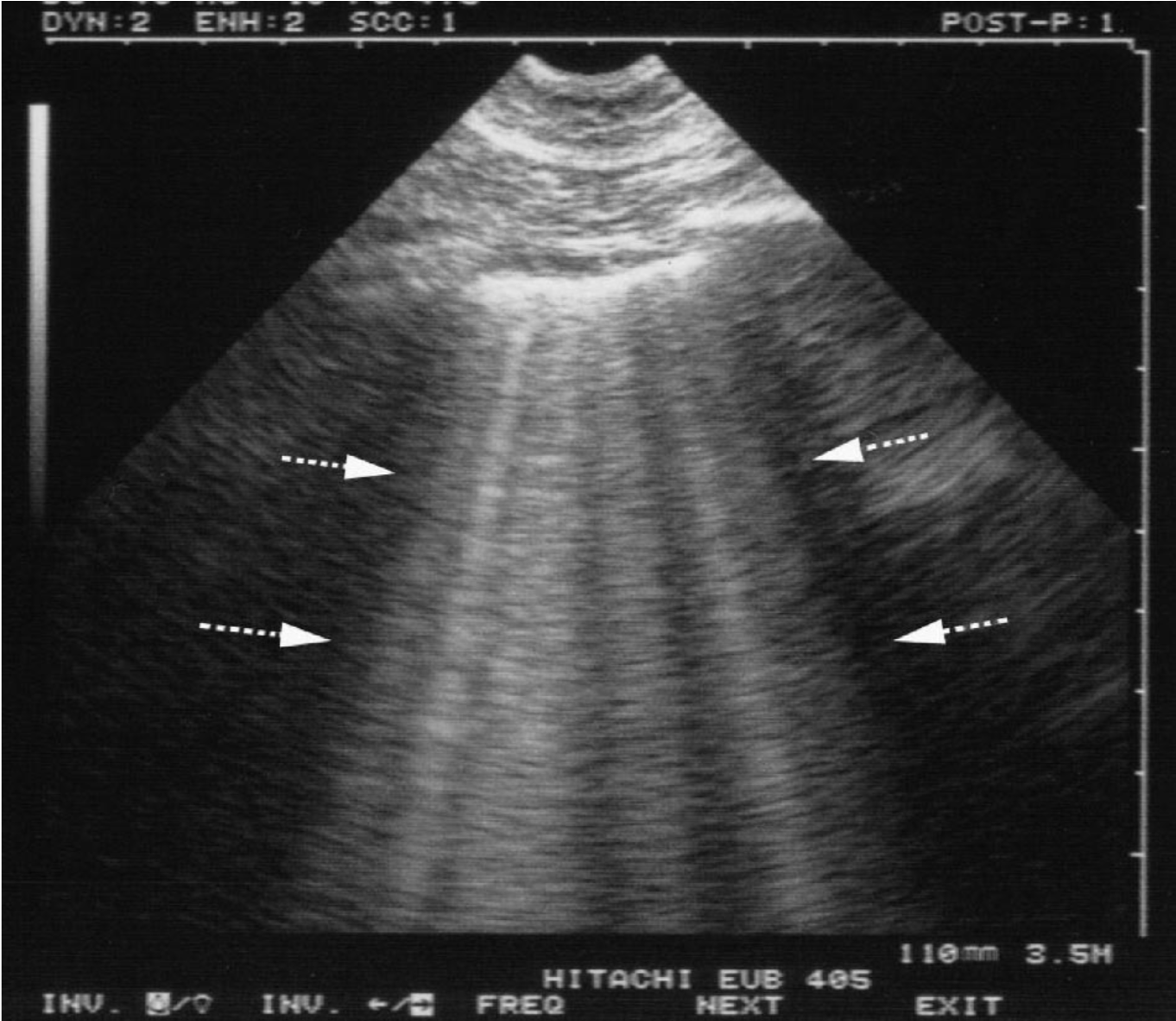
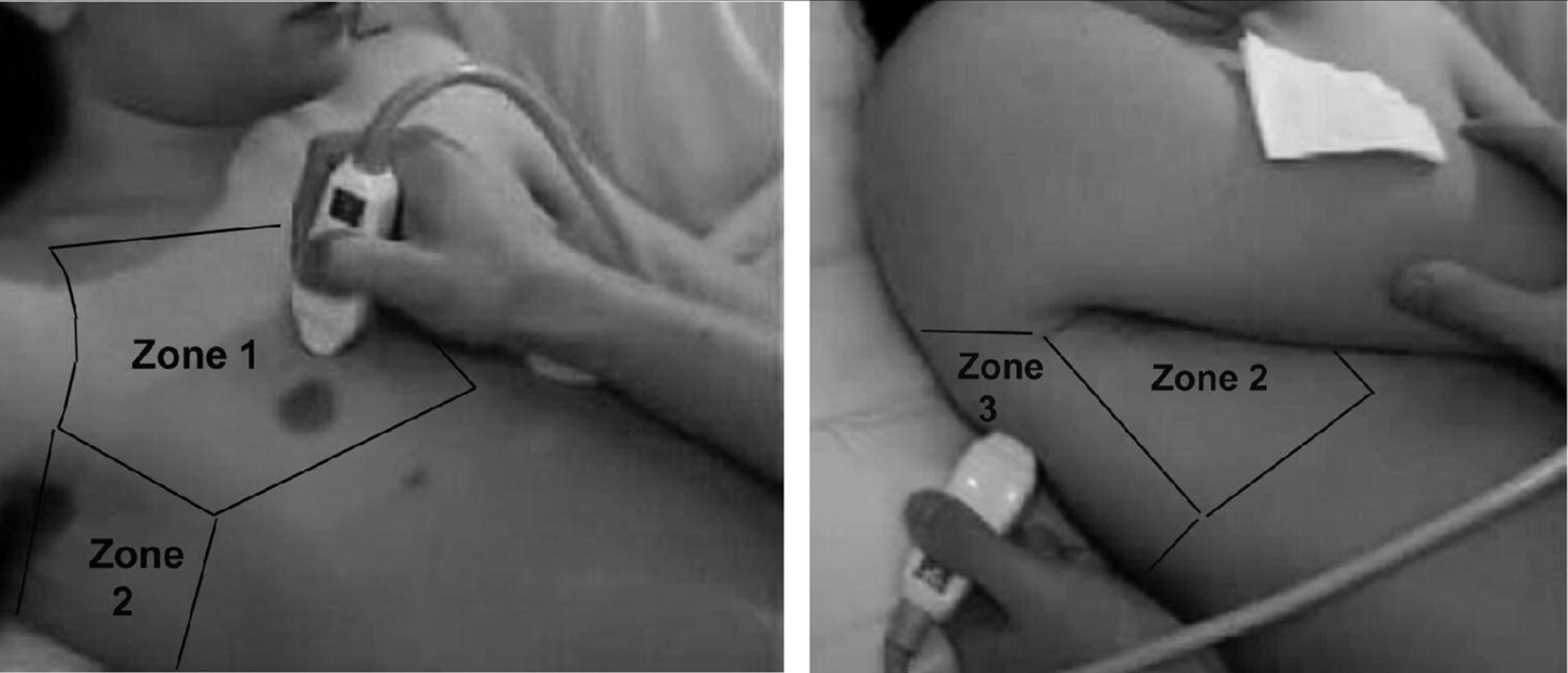
Mar 22, 2019 Explore the intricacies of acute decompensated heart failure in the ED. Learn how to identify key features that indicate heart failure and the significance of B-lines in pulmonary edema. The discussion dives into using ultrasound techniques and ECG to aid diagnosis. Additionally, discover the role of BNP testing and effective management principles, including diuretic dosing and strategies for addressing both redistribution and fluid overload. The insights shared are essential for improving patient outcomes in urgent situations.
AI Snips
Chapters
Transcript
Episode notes
Definition And Diagnostic Importance
- Acute decompensated heart failure includes impaired filling or reduced ejection fraction and is common in the ED.
- Missing the diagnosis may increase mortality, so clinical suspicion matters.
History And Exam Predictors
- Certain history and exam findings strongly increase the probability of heart failure, including prior CHF, PND, orthopnea, and DOE.
- An S3 had a very high positive likelihood ratio, followed by JVD and rales.
Always Get An ECG
- Always obtain an ECG to assess for acute myocardial infarction in dyspneic patients.
- A normal ECG makes left ventricular systolic dysfunction unlikely, with a high negative predictive value.